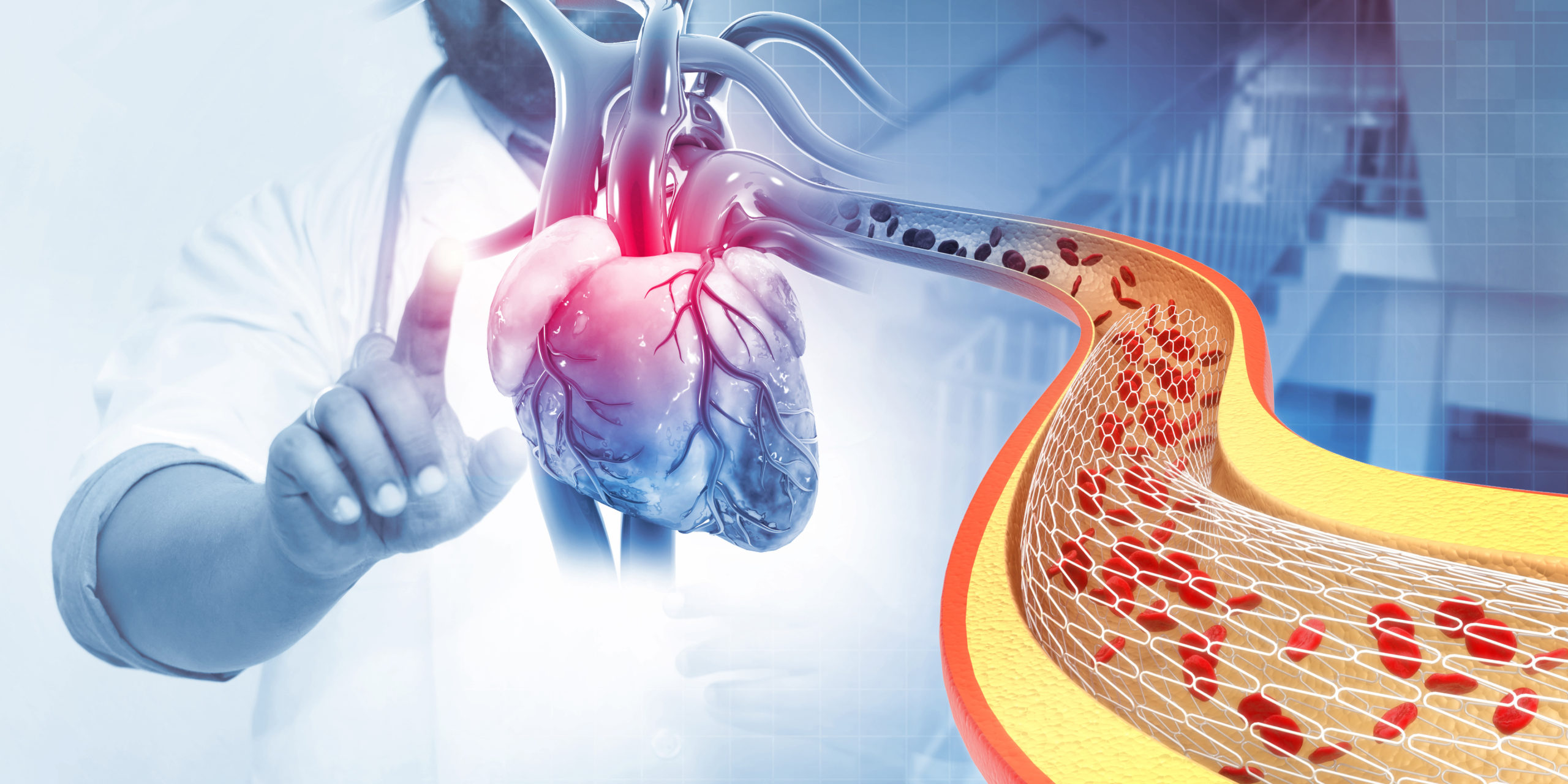
Nutrition plays an enormous role in heart attack and post-stent recovery and in the prevention of further heart health complications. If you or someone you know has been in this situation, you may be wondering what type of diet after a heart attack and stents has proven beneficial.
As a cardiology dietitian, I’ve met with countless individuals in this situation. When a stent is placed or you experience a heart attack, it can feel like information overload. I’m here to empower you to take control of your health and make sustainable lifestyle changes.
I want to start by telling you a story.
A Success Story
I continue to be mind blown by so many of my clients’ results as we work together. One such client exemplifies just how powerful science-based nutrition can be for recovery from heart attacks and stents.
A 44-year-old gentleman came to see me after three heart attacks and six stent placements. He had changed his diet on his own multiple times but was confused about what he was “doing wrong” that was continuing his cardiovascular complications. His doctor told him he would have to return in a month for his 7th stent.
We began working together to optimize his labs. He started with an LDL cholesterol of 95mg/dL, which is high for a heart attack survivor who is also on a statin. He also had a non-HDL cholesterol (an indication of atherogenic apoB cholesterol) of 113mg/dL. These numbers should be less than 50mg/dL and less than 80 mg/dL in heart attack survivors, respectively.
To target these labs, we added therapeutic foods to optimize his blood vessel health and reduce inflammation. After 1.5 months, he returned to his doctor who then said he no longer needed that 7th stent!
His new lab results showed an LDL of 41mg/dL and a non-HDL cholesterol of 54mg/dL. My client stated how much more energy he has now. He doesn’t remember ever feeling this good — and I am so proud of him.
That’s the power of science-based nutrition. It can absolutely turn your life around, even after multiple heart attacks and stents.
What is a Stent?
A stent is a tube surgically placed into your arteries to help keep them open. Arteries are the blood vessels that transport blood from your heart to the rest of your body. When clogged with plaque, blood flow slows, which is coronary artery disease (CAD). This can ultimately cause a blood clot that triggers a heart attack.
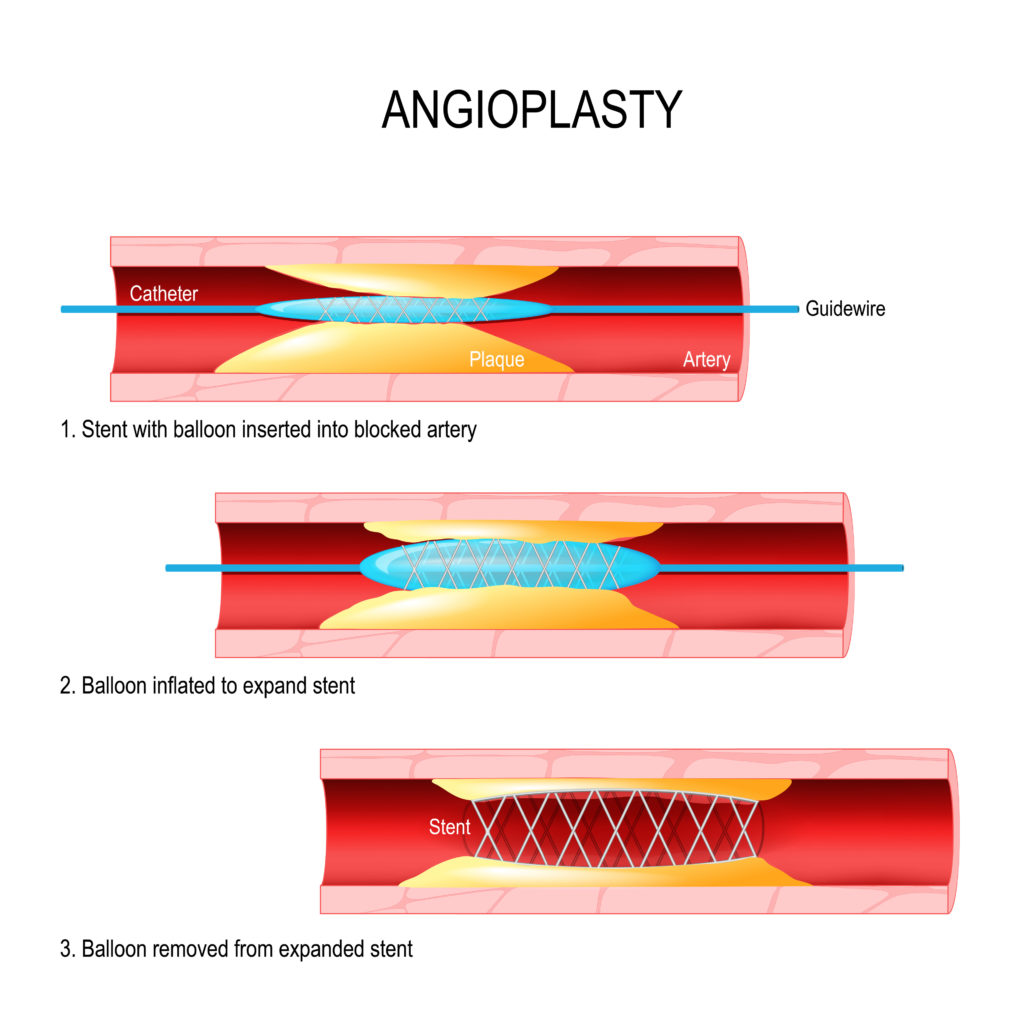
While a stent may prevent or stop a heart attack that’s already happening, it’s not a cure for CAD. Making other lifestyle changes after receiving a stent, or having a heart attack — like a nutrition overhaul — are critical for continued health.
Diet After Heart Attack and Stents
My aforementioned client had tried making nutrition changes on his own before. And while his intentions were good, he ended up having his second heart attack as a result — despite taking all of his prescribed medications. But what was he doing wrong?
Well, first let’s talk about the goals of diet after a heart attack. A nutrient sufficient heart healthy diet goals should focus on:
- Stabilizing the plaque already present in your arteries
- Preventing further promotion of plaque
- Reducing the overtaxing on the heart to allow it to optimally function to prevent heart failure, heart enlargement, and heart pumping complications.
- Optimizing all the risk factors you may have, such as lowering LDL and non-HDL cholesterol, hs-CRP inflammation markers, insulin resistance, and waist circumference
- Addressing the underlying root causes of heart disease, like inflammation, oxidative stress, insulin resistance, overweight or obesity, and plaque buildup
The reason the diet changes my client made before meeting with me didn’t work was that they didn’t do any of the things on this list. In fact, the changes made all of these factors worse, furthering the progression of his plaque buildup and arterial blockages, hence leading to another heart attack.
What Should I Eat After a Stent?
As with any other health goal, there’s never one single food that makes all the difference. It’s the cumulative effect of many foods that helps.
In general, this means an abundance of minimally-processed foods, like polyphenol rich fruits, nitric oxide, folate rich vegetables, whole grains, legumes, nuts, seeds, and lean proteins. Furthermore, I like my clients, including this gentleman, to keep a few things in mind.
1. Carbohydrates aren’t the enemy.
Cutting carbs isn’t the answer. Low-carb diets ignore the fact that carbs are actually super important for your health — it’s just that many people aren’t eating many of the right ones.
Rather than just restricting carbohydrate-containing foods with little nutritional value, low-carb diets tend to minimize the whole range of carbohydrates, including nutrient-dense sources like fruits, vegetables, whole grains, and legumes.
Healthy carbs provide energy and fiber, an important nutrient that many people are lacking that can help reduce high cholesterol and heart disease risk.
2. Add more polyphenols.
Polyphenols are compounds found in plants that act like antioxidants. They help protect your body from free radicals that cause cellular damage. Eating them may help improve multiple heart disease risk factors, like reducing blood pressure and LDL, while raising HDL.
Some sources of polyphenols include cocoa powder, berries, plums, artichokes, hazelnuts, cloves, and black tea.
3. Boost your nitric oxide intake.
Many people who have plaque in their arteries also have less nitric oxide. Nitric oxide is a molecule that promotes the dilation of the blood vessels, supporting healthy circulation.
Some foods that help increase nitric oxide include beets and greens like spinach, arugula, and kale.
4. Ditch Paleo.
The Paleo diet is presumed to mimic the way the cavemen ate, although that’s up for debate. This is the diet my client switched to after his first heart attack, unknowingly worsening his heart health.
It’s easy to get caught up in the red meat-heavy aspect of Paleo. Recent research has found that red meat and foods high in choline and carnitine can promote the production of a compound called trimethylamine N-oxide (TMAO). Higher levels of TMAO are associated with plaque buildup and heart disease.
5. Remove other foods that contribute to poor heart health.
Again, no single food causes a heart attack, but understanding the types of foods that promote them can help you avoid these in your diet.
These include:
- Ultra-processed foods are made with no or minimal whole foods ingredients and have undergone significant processing to make them convenient, hyper-palatable, and appealing. Frequent consumption can cause high levels of cystatin C, a protein used as a biomarker for kidney function and premature cardiovascular death. Examples include prepared soups, sauces, ready-to-eat meals, frozen pizza, store-bought cookies, and more.
- Soda and similar beverages provide calories from added sugar but no real nutrition.
- Foods cooked at high temperatures. Swap these for cooking methods like stewing, braising, and roasting to reduce advanced glycation end products (AGEs) that otherwise promote oxidative stress, inflammation, and heart disease.
Designing a Heart Healthy Plan
The right diet after a heart attack and stents will follow the recommendations above. But in order to see success like my clients, a plan will also take into account your lifestyle and cultural preferences and other individual factors to encourage long-term sustainability. To design a meal plan that will work for you, it’s important to understand the science-based nutrition behind it.
Need some help? I’d love to invite you to join my 6-week Heart Optimization Group Program! If you want a more personalized approach, feel free to learn more about my 1:1 counseling and schedule a complimentary discovery call to discuss further.
References
- Soliman GA. Dietary Fiber, Atherosclerosis, and Cardiovascular Disease. Nutrients. 2019;11(5):1155. Published 2019 May 23. doi:10.3390/nu11051155
- Cory H, Passarelli S, Szeto J, Tamez M, Mattei J. The Role of Polyphenols in Human Health and Food Systems: A Mini-Review. Front Nutr. 2018;5:87. Published 2018 Sep 21. doi:10.3389/fnut.2018.00087
- Król M, Kepinska M. Human Nitric Oxide Synthase-Its Functions, Polymorphisms, and Inhibitors in the Context of Inflammation, Diabetes and Cardiovascular Diseases. Int J Mol Sci. 2020;22(1):56. Published 2020 Dec 23. doi:10.3390/ijms22010056
- Hord NG, Tang Y, Bryan NS. Food sources of nitrates and nitrites: the physiologic context for potential health benefits. Am J Clin Nutr. 2009;90(1):1-10. doi:10.3945/ajcn.2008.27131
- Zeisel SH, Warrier M. Trimethylamine N-Oxide, the Microbiome, and Heart and Kidney Disease. Annu Rev Nutr. 2017;37:157-181. doi:10.1146/annurev-nutr-071816-064732
- Bonaccio M, Costanzo S, Di Castelnuovo A, et al. Ultra-processed food intake and all-cause and cause-specific mortality in individuals with cardiovascular disease: the Moli-sani Study. Eur Heart J. 2022;43(3):213-224. doi:10.1093/eurheartj/ehab783
- Deo R, Sotoodehnia N, Katz R, et al. Cystatin C and sudden cardiac death risk in the elderly. Circ Cardiovasc Qual Outcomes. 2010;3(2):159-164. doi:10.1161/CIRCOUTCOMES.109.875369
- Uribarri J, Woodruff S, Goodman S, et al. Advanced glycation end products in foods and a practical guide to their reduction in the diet. J Am Diet Assoc. 2010;110(6):911-16.e12. doi:10.1016/j.jada.2010.03.018
- Willemsen S, Hartog JW, Heiner-Fokkema MR, van Veldhuisen DJ, Voors AA. Advanced glycation end-products, a pathophysiological pathway in the cardiorenal syndrome. Heart Fail Rev. 2012;17(2):221-228. doi:10.1007/s10741-010-9225-z