The two conditions – heart attack and heart failure – sound similar, but they are not the same thing. Understanding what distinguishes a heart attack from heart failure is easy to understand. In this article you’ll learn:
- What are heart attacks and heart failure?
- How are they different?
- How can you prevent future recurrences?
Those questions are exactly what this article will answer for you.
What is the heart and what does it do?
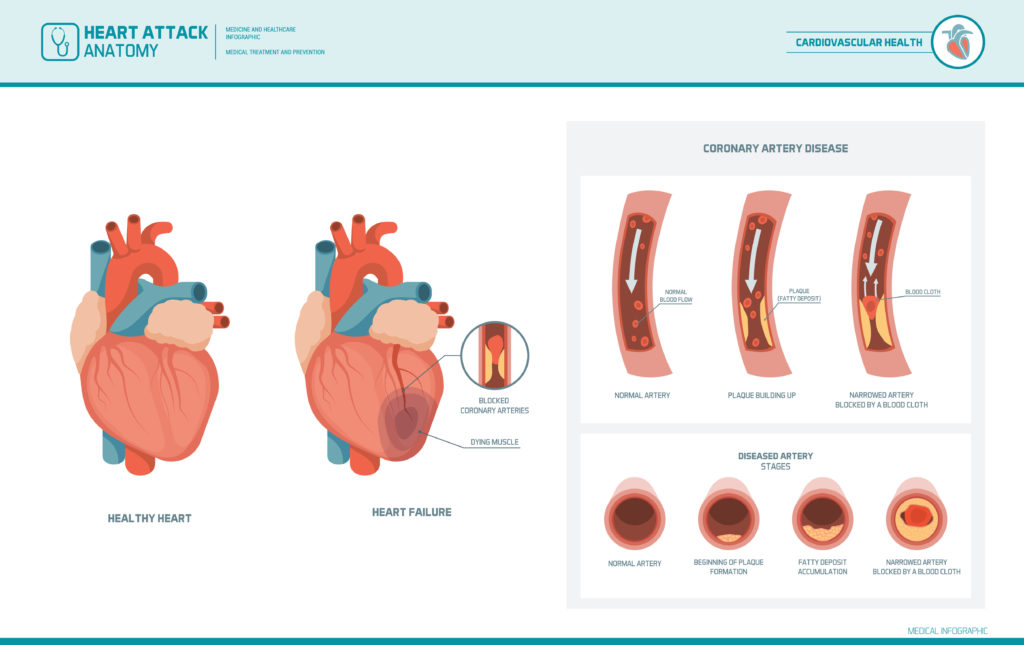
The heart is a muscle in your chest that pumps blood through your entire body. It sits between the lungs and slightly to the left of the center of the chest. The heart contains a right side and four chambers — two on the top and two on the bottom.
The contraction of the atria and ventricles results in the heart pumping and produces the heartbeat. As your heart pumps, blood moves through the body carrying nutrients and oxygen to all of the cells of your body and carrying away waste products.
The two upper chambers, the atria, are the smaller chambers. The two lower chambers, the ventricles, are the larger chambers.
When the heart beats, the atria contract moving blood into the ventricles. This is the first part of the heartbeat that is a bit quieter. The second, louder beat happens when the ventricles contract. The contraction of the ventricles moves the blood out of the heart and to the lungs from the right ventricle, and to the body from the left ventricle.
If you want to see a visual of the heart pumping, the Children’s Hospital of Philadelphia has a great video with explanations of the different parts of the pumping action if you want to understand more how the heart works.
What is a heart attack?
A heart attack happens when one or more of the arteries that supply blood to the heart becomes blocked.
As a result of the blood flow being blocked, the heart will beat irregularly. If the blood flow is not restored quickly, that part of the heart muscle can die. If part of the heart muscle dies, scar tissue forms. This damage to the muscle means that the heart will not pump as well as it did prior to the heart attack. The technical term for a heart attack is a myocardial infarction.
Knowing the symptoms of a heart attack can help you react quickly if you think you, or someone you love, is having one.
What are the symptoms of a heart attack?
Most importantly, if you or someone you know experiences any of the symptoms, help should be sought immediately – call 911 or get the person to the emergency room as quickly as possible.
The five most common symptoms of a heart attack4, 6 are:
- Discomfort in the jaw, neck, or back
- Weakness or lightheadedness
- Chest pain or discomfort
- Chest pain that travels from the left arm to the neck
- Arm or shoulder discomfort
- Shortness of breath with or without chest pain
- Sweating
- Nausea
- Vomiting
- Abnormal heartbeat
Women may experience different symptoms than men. Women are more likely to experience5:
- Chest pain that is sharp, burning, aching, or like a soreness
- Unusual fatigue
- Unusual shortness of breath
- Upper back/chest pain
- Neck, jaw, arm, shoulder, or back pain
- Pain in the upper stomach, immediately below the ribs
- Flu-like symptoms
- Dizziness
- General feeling of scaredness or anxiety
- General feeling of weakness
- Indigestion
Next, let’s talk about what causes a heart attack and how you can prevent one from happening in the first place.
What causes a heart attack?
The leading cause of a heart attack is the development of atherosclerosis, or plaque buildup, in the arteries that surround the heart. Atherosclerosis can happen in any of your arteries or blood vessels throughout the body. However, when it happens in the arteries of the heart then it can lead to a heart attack.
Other causes of a heart attack include5:
- An artery of the heart spasming
- Spontaneous Coronary Artery Dissection – when there is a tear in one of the arteries of the heart
A heart attack can be a stand-alone event, or it may lead to heart failure.
Now that we’ve covered heart attacks, we’ll cover what heart failure is and what distinguishes a heart attack from heart failure.
What is heart failure?
Heart failure isn’t what it sounds like – that the heart has stopped working. What heart failure really means is that the heart isn’t working as well as it could.
In reality, heart failure develops over time for a variety of reasons (more about why heart failure develops below). Because the heart muscle isn’t working as well as it used to, it makes adaptations to try to keep up with the workload.
For example, some of the adaptations your heart makes include:
- Enlarging: the heart, particularly the left ventricle gets bigger in an attempt to produce a greater contraction and to pump more blood to the body.4
- Increasing muscle mass: Your heart builds more muscle to attempt to contract more strongly. This can help for a while.4
- Contracting more frequently: This results in a rapid heart rate because the heart is trying to keep up by contracting more times each minute than it used to.4
Not surprisingly, the heart isn’t the only part of the body that tries to make changes. Blood arteries and vessels throughout the body will narrow to compensate for the heart’s lower strength contractions.4 This can be a problem if some of the arteries and vessels are narrowed due to atherosclerosis. They become easier to be blocked.
Another adaption the body makes is to reduce blood flow to areas of the body, including tissues, and organs that are less important than the heart.5
Only when these compensations and adaptations stop working do you start to feel symptoms. The progression of heart failure can take years until you start feeling the symptoms.
If you aren’t sure if you’re experiencing heart failure or have concerns about your heart, you can talk with a cardiologist. They can test your heart’s ejection fraction by having an echocardiogram performed. These tests will give you the information you need about how efficiently your heart is working.
Next, we’ll cover the causes of heart failure.
What causes heart failure?
Heart failure has multiple causes and usually develops over a period of time. Below is a list of some things that can cause heart failure6:
- Heart attack: a heart attack causes some of the heart muscle to die and leaves behind scar tissue. This decreases the ability of the heart to contract and pump blood.
- Coronary artery disease and cardiovascular disease: When the arteries that provide blood to the heart muscles are narrowed with plaque.
- Heart valve disease: If the heart valves aren’t working properly. This can be caused by rheumatic fever or other infections.
- Hypertension (AKA high blood pressure): The heart has to work harder to pump blood when blood pressure is high.
- Complications of diabetes
While the causes are straightforward, the symptoms of heart failure can be vague. In the next section, the symptoms of heart failure are covered.
What are the symptoms of heart failure?
Here is a list of the most common symptoms of heart failure. If you’re experiencing heart failure, you may:
- Feel short of breath when resting, during exercise, or even when lying flat.
- Have swelling in the abdomen, legs, and ankles due to a buildup of fluid.
- Be tired and weak.
- Experience a loss of appetite, nausea, and abdominal pain.
- Gain weight.
- Have a cough that produces blood-tinged sputum.
Is Heart Failure Reversible?
For most people, heart failure progresses over a number of years. And, its progression can be slowed and even reversed. This is good news!
So, how do you reverse it?
The best way to reverse heart failure is to address the underlying problems like taking steps to reduce cardiovascular disease and atherosclerosis. Getting other health issues like high blood pressure and diabetes under control is also critical to reversing the progression of heart failure.
If you have any arteries that are partially or completely blocked, having one of the available surgical procedures can open them up so that your heart gets the blood and nutrients it needs.
If you have abnormal heart rhythms, those should be treated, too.
Another way to minimize your risk for heart failure is to address lifestyle factors including:
- What you eat
- Stress management
- Stopping smoking if you’re a smoker
- Reducing alcohol intake.
Although “watching what you eat” sounds simple, it is more than just watching your salt.
Following a scientifically-based nutrition program that targets the risk factors for developing a heart attack or heart failure can help keep you, and your heart, healthy. We’ll talk more about a science-based nutrition program below.
What distinguishes a heart attack from heart failure?
To summarize:
- A heart attack is when part of the heart loses blood flow.
- Heart failure is when the heart can’t pump as effectively as it used to.
Both reduce the heart’s ability to pump blood through the body.
What is cardiovascular disease and how does it contribute to heart attacks and heart failure?
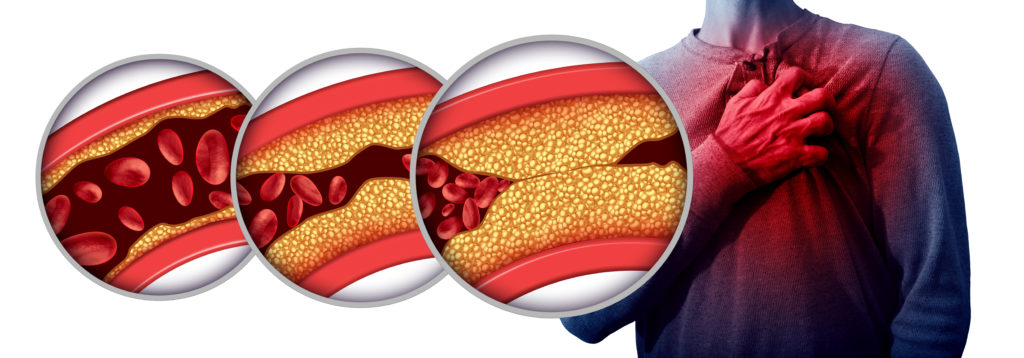
Cardiovascular disease (CVD) plays a role in both heart attack and heart failure. CVD is an umbrella term for disorders of the heart and blood vessels. Furthermore, atherosclerosis is the major cause of cardiovascular disease1.
Atherosclerosis causes a narrowing and stiffening of arteries and vessels in the body and in the heart. The buildup that causes the narrowing and stiffening is called plaque.
This plaque develops when there is an injury to the inside of a blood vessel. LDL particles from the bloodstream put cholesterol at the site of the injury. This sets off the inflammatory response and the body’s immune system gets called into action. This process is described in my blog post What a High LDL Particle Number Means for Developing Atherosclerosis.
The main cause of heart attacks is when either the plaque or the cap are unstable and break off – a clot. The clot travels through the bloodstream until it reaches a narrow part of the blood vessel or artery and causes it to clog and stop the flow of blood beyond where the clot happened.
Atherosclerosis leads to heart failure when the arteries that lead to the heart become narrowed and stiff due to plaque buildup. This causes the heart to not get as much blood flow, nutrients, and oxygen which means the heart may not pump as well as if the arteries did not have plaque buildup. As mentioned previously, a heart attack, also caused by atherosclerosis, can lead to heart failure.
You’ve been told you’ve had a heart attack or heart failure. Now what?
If your doctor tells you you’ve had a heart attack or heart failure, you want to know how to fix it. As a Registered Dietitian who specializes in heart disease and who has worked with thousands of patients in your shoes, I want you to know that there are things you can do to help your heart keep beating for years to come.
Having a diet that gives your body, and your heart, what it needs is more than just following a low sodium diet for heart failure. Here are five things I recommend to my clients who have had heart attacks or who have heart failure, or both.
- Know your numbers including your blood pressure, your Hemoglobin A1c, fasting insulin, your LDL particle number, small LDL size, and ejection fraction percentage. Optimize these values to assist with blood vessel health protection.
- Eat potassium-rich foods. Potassium has been shown to relax the blood vessels and lower blood pressure. The recommended intake for potassium for men ages 19-50 is 3,400 mg/day and 2,600 mg/day for women. If you have cardiovascular disease, the recommendation goes up to 4,700 mg/day. Potassium-rich foods include dried apricots (550 mg in 1/4 cup), a medium baked potato (610 mg), and a medium banana (422 mg). Avoid high dose Potassium supplements due to its side effects of cardiac arrhythmias and intestinal bleeding.
- Ensure nutrient sufficiency. One of the biggest things I find with my clients is that they have nutrient deficiencies. Multiple research studies also show those with heart failure and heart attacks aren’t getting enough vitamins and minerals.2, 3 For example, over 20% of people with heart failure aren’t getting enough Vitamin A, calcium, magnesium, selenium, iodine, and Vitamin D in their diet. Rather than looking for supplements that can have fillers and synthetic agents that can increase inflammation, use food first.
- Be informed about your medication and its ability to lower or retain certain nutrients from your body. Some medications prescribed for heart failure can actually deplete some of the key nutrients your body needs for optimal heart health. This can have the effect of making heart failure worse. Checking your medications to see if they impact your vitamin and mineral status can help you figure out what additional foods to add to your meals.
- Address Oxidative Stress. Research shows that those with heart failure have more oxidative stress. How you eat can either increase or decrease the oxidative stress in your body. For example, you want to optimize the production of glutathione which helps reduce oxidative stress. Eating vegetables that include allium, like garlic, shallots, and leeks gives your body what it needs to produce glutathione.
Heart attacks and heart failure are complex conditions. Searching Dr. Google gives you a lot of information, but you have to put all of the pieces together. You don’t have to do it alone!
Get Personalized Help with Your Heart Healthy Diet

If you want a trusted, personalized, science-based program that hundreds of people have gone through and improved their heart health, you can sign up for one-on-one counseling with me. Together, we’ll work to manage your risk factors and implement a nutrient-sufficient, heart-healthy diet that optimizes your cardiovascular function.
Nutrient sufficiency is an often overlooked aspect of nutrition planning. Rather than just eating enough fruits and vegetables, we’ll work together to ensure you’re getting the right amounts of lean proteins, healthy fats, complex carbohydrates, therapeutic foods, and vitamins and minerals your body needs.
You can schedule a time to talk with me about your needs and we can choose the right program for you. To learn more about my programs offered, feel free to review this page on my website.
