If you’ve been diagnosed with peripheral artery disease, you’re probably wondering how much your diet really matters. As a cardiovascular dietitian with over 14 years of experience, I can tell you that a personalized, science based approach is one of the most powerful tools you have. And I want to share a story that shows you exactly what’s possible.
A 55-year-old woman came to see me recently because she was struggling with constant leg pain and difficulty walking. Looking over her labs and medical history, it was apparent she was dealing with elevated blood pressure (130/80mmHg), high blood sugar levels (103mg/dL), high LDL cholesterol (130mg/dL), and an increased waist circumference of 39 inches, an indication of metabolically active adipose tissue that increases the risk of fat accumulation around the heart. She’d already been put on medications and told to follow a heart healthy diet, but she wasn’t seeing relief.
After a comprehensive 90-minute evaluation of her nutrition, lifestyle, and medical history, we built a personalized, anti-inflammatory nutrition plan. It focused not on cutting foods out, but adding the right ones in, in the right amounts and pairings for her needs.
Within 3 weeks, her blood pressure improved to 112/72mmHg and her leg inflammation began to subside. Within six weeks, her energy increased and her circulation noticeably improved.
Her story is possible for you, too. A personalized peripheral artery disease diet can help reduce symptoms, improve blood flow, and protect your long-term vascular health.
In this blog, I’ll walk you through exactly how science based nutrition can make a meaningful difference for PAD.
What is Peripheral Artery Disease?
To understand how diet can make a difference, it helps to first understand what PAD actually is and what’s driving it.
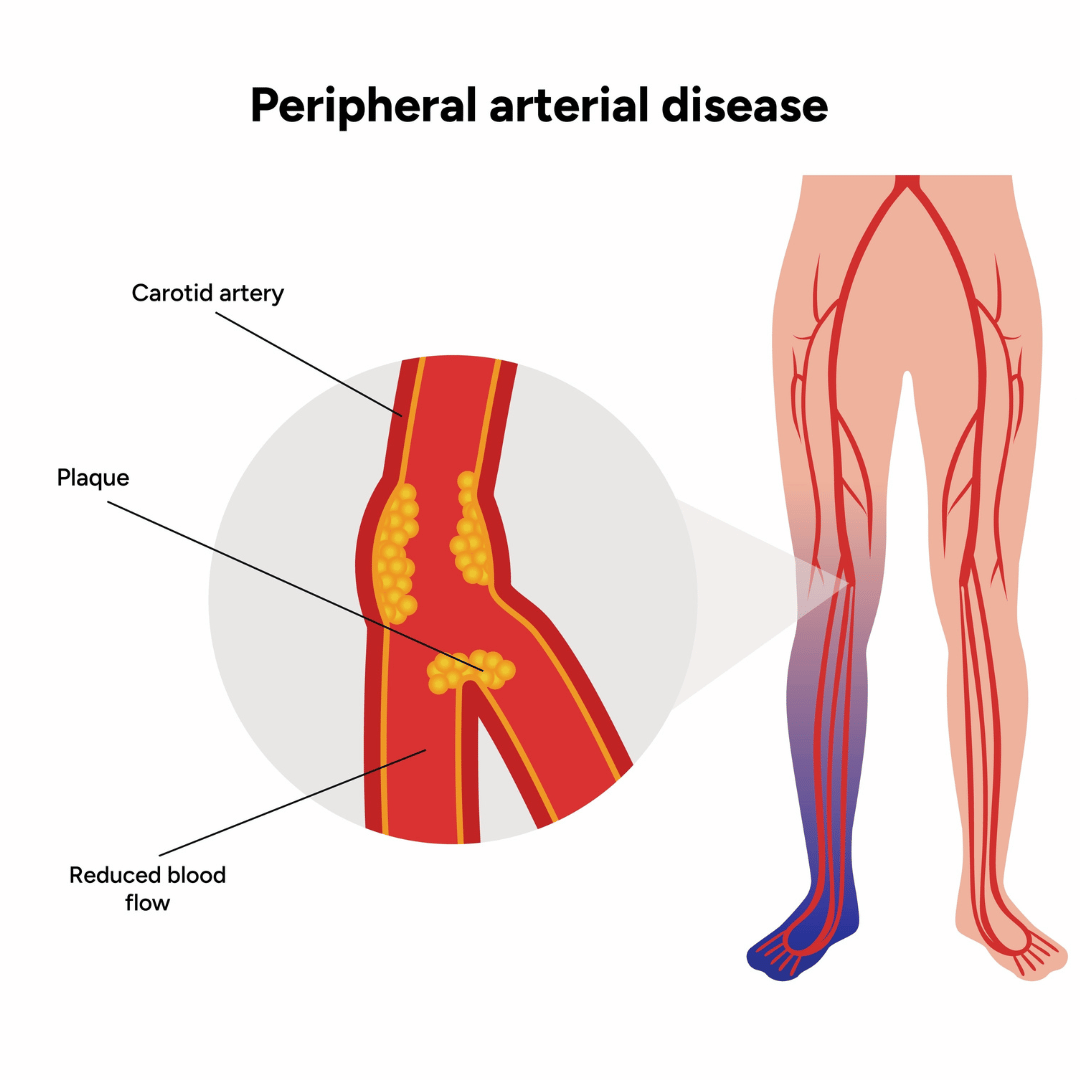
Peripheral artery disease (PAD) is a circulatory condition caused by plaque buildup in the arteries of your lower extremities. This leads to narrowing of the arteries and reduced blood flow to your legs and feet.
Just like plaque can build up in your coronary arteries and raise your risk of heart attack, it can also build up in the arteries of your legs and feet. PAD is essentially the same disease process happening in a different part of your body.
Research shows that people with PAD have up to a 68% higher risk of ischemic heart disease compared to those without it, as well as significantly elevated risk of heart failure and other vascular events.
Common Symptoms of PAD
- Cramping or aching in the legs during walking or physical activity that goes away when you stop
- Numbness, weakness, or heaviness in the lower legs or feet
- Feet or lower legs that feel consistently cold to the touch
- Wounds on the feet or legs that are slow to heal or won’t heal at all
- Changes in skin color, texture, or hair growth on the legs and feet
Some people with mild PAD have no symptoms at all, which makes it easy to overlook until it progresses.
Modifiable Risk Factors of PAD
The good news is that many of the risk factors that drive PAD are modifiable. A personalized, science based nutrition approach that targets your individual risk factors gives you a real opportunity to improve blood flow, reduce symptoms, and protect your long term heart health.
- Smoking (the strongest modifiable risk factor)
- High blood pressure
- High cholesterol
- Elevated blood sugar levels and diabetes
- Obesity and sedentary lifestyle
How Does Diet Affect Peripheral Artery Disease?
The foods you eat daily play a role in the progression of PAD. Here are a few of the ways a peripheral artery disease diet can make a difference:
- Reduce chronic inflammation: Following an anti-inflammatory diet that supports gut health, promotes blood flow, and meets your nutrient needs helps to lower the inflammatory response that drives plaque buildup and arterial damage in PAD.
- Support endothelial health: The endothelium is the inner lining of your arteries. Specific nutrients, in the right amounts and pairings, support its ability to produce nitric oxide, which keeps arteries flexible, reduces arterial stiffness, and promotes efficient blood flow to the lower extremities.
- Improve blood sugar and insulin sensitivity: Chronically elevated blood sugar damages arterial walls and accelerates atherosclerosis. Strategic macronutrient balance, food pairings, and meal timing can meaningfully improve insulin sensitivity and protect vascular health.
- Optimize cholesterol and blood pressure: Atherogenic LDL cholesterol fuels plaque buildup directly inside the arterial walls, and elevated blood pressure accelerates the damage by increasing stress on those walls. Targeted nutrition can meaningfully lower both, reducing two of the most significant drivers of PAD progression.
- Combat oxidative stress: Oxidative stress damages arterial walls and worsens circulation. Specific antioxidant pathways in the body can be supported through food to protect vascular health long term.
A peripheral artery disease diet isn’t about restriction. It’s about consistently meeting your nutrient needs, optimizing your cardiometabolic metrics, reducing the havoc in your bloodstream, and slowing plaque progression in the femoral arteries so you can protect your vascular health and improve your quality of life long term.
The Best Peripheral Artery Disease Diet
The best peripheral artery disease diet is one that’s focused on nutrient adequacy and personalized to your individual labs, medical history, and cardiovascular risk factors.
Personalization is what makes it sustainable, because when we optimize your cardiometabolic metrics, meet your nutrient needs, and stabilize plaque, we’re building a foundation that protects your vascular health for the long haul.
The goal of a science-based, personalized nutrition approach for PAD is to improve blood flow, halt new plaque progression throughout the entire vascular system, and to support the regression of soft plaque that hasn’t yet hardened.
The good news is that the right nutrition can meaningfully move the needle on all three of these goals, and research gives us a strong foundation to work from.
Research consistently supports the Mediterranean diet as a strong starting point for a peripheral artery disease diet, effective for both prevention and management. Within that framework, though, there’s important nuance. The right amounts, food sources, and pairings will depend entirely on your individual labs, health history, and cardiovascular risk factors.
Mediterranean Diet for Peripheral Artery Disease
The Mediterranean Diet is a flexible, sustainable way of eating built around whole, minimally processed foods. Here’s what to focus on:
- Fruits and Vegetables: Leafy greens, tomatoes, peppers, berries, citrus, and seasonal produce. These provide the antioxidants and anti-inflammatory compounds your arteries need.
- Whole Grains: Oats, brown rice, quinoa, and whole grain bread over refined carbohydrates. These support healthy blood sugar and provide soluble fiber that benefits cholesterol and circulation.
- Legumes: Lentils, chickpeas, and beans several times a week. These are rich in fiber, plant protein, and nutrients that support vascular health.
- Healthy Fats: Extra virgin olive oil is the cornerstone of the Mediterranean diet and has well documented benefits for endothelial function and inflammation. Nuts and seeds are also key.
- Fish and seafood at least twice a week, particularly fatty fish like salmon, sardines, and mackerel, which are rich in omega-3 fatty acids that support blood flow and reduce inflammation.
- Lean proteins like poultry, eggs, and low-fat dairy in moderation, with red and processed meat kept to a minimum.
While the Mediterranean diet provides a strong evidence-based starting point, the real results come from personalizing that framework to your specific labs, risk factors, and health history. If you’re ready to take a targeted, science-based approach to protecting your vascular health, my group program Optimize was built exactly for that.
Best Foods for Peripheral Artery Disease
In my practice, I use a food first approach. These six research backed nutrients can be found in everyday foods, and they’re the ones that matter most for PAD. Keep in mind that the right amounts for you will depend on your unique cardiovascular picture.
- Omega-3 Fatty Acids: These healthy fats reduce inflammation, support endothelial function, and help improve circulation throughout the vascular system. Food sources include fatty fish like salmon, sardines, and mackerel, as well as walnuts, flaxseeds, and chia seeds.
- Polyphenols: These are plant compounds that protect arterial walls, support nitric oxide production, and help slow plaque progression. Food sources include extra virgin olive oil, berries, dark leafy greens, green tea, and dark chocolate.
- Soluble Fiber: Soluble fiber binds to cholesterol in the digestive tract, helping to lower atherogenic LDL levels, blood sugar, and blood pressure, all key drivers of PAD progression. Food sources include oats, lentils, beans, apples, barley, and flaxseeds.
- B Vitamins (Folate, B6, B12): B vitamins help regulate homocysteine levels, and elevated homocysteine is associated with increased arterial stiffness and vascular inflammation in PAD. Food sources include leafy greens, lentils, chickpeas, eggs, salmon, and fortified whole grains.
- Dietary Nitrates: Nitrates support nitric oxide production, which keeps arteries flexible and improves blood flow to the lower extremities. Food sources include beets, spinach, arugula, Swiss chard, and celery.
- Vitamin D: Low vitamin D levels are associated with PAD prevalence and severity. Food sources include fatty fish, egg yolks, fortified dairy, and mushrooms exposed to sunlight.
These nutrients have strong research support for vascular health. But the right amounts, food sources, and combinations for you depend on your labs, medical history, and cardiovascular risk factors.
Can Peripheral Artery Disease Be Reversed With Diet?
This is one of the most common questions I hear, and I want to give you an honest answer.
Diet alone can’t fully reverse established PAD. But in my 14 years of working with clients, I’ve seen firsthand how much is possible when nutrition is truly personalized and science based. Life changing improvement is possible.
Think back to the client I mentioned at the start of this article. She came in with constant leg pain, elevated blood pressure, high cholesterol, and high blood sugar. Within three weeks of implementing a targeted, anti-inflammatory nutrition plan, her blood pressure improved from 130/80 to 112/72mmHg and her leg inflammation began to subside. Within six weeks her energy increased and her circulation noticeably improved.
Those changes were life changing for her.
Here’s what targeted nutrition can achieve with PAD:
- Reduced leg pain and improved walking capacity
- Improved blood flow and endothelial function
- Slower plaque progression throughout the vascular system
- Soft plaque regression with consistent, targeted nutrition
- Improved cholesterol, blood pressure, and blood sugar levels
- Reduced systemic inflammation, a key driver of PAD progression
- Meaningfully reduced risk of heart attack, stroke, and increased quality of life
How much improvement is possible depends on the stage of your disease, your individual risk factors, and how targeted your nutrition approach is. A personalized, nutrient adequate peripheral artery disease diet that addresses the underlying root causes of your PAD can get you relief.
FAQs: Peripheral Artery Disease Diet
What foods help peripheral artery disease?
Foods rich in omega-3 fatty acids, polyphenols, soluble fiber, dietary nitrates, B vitamins, and vitamin D are the most well supported for PAD. Focus on fatty fish, extra virgin olive oil, leafy greens, berries, legumes, whole grains, and nitrate-rich vegetables like beets and spinach.
What is the best diet for peripheral artery disease?
Research supports a Mediterranean-style eating pattern as the foundation for a PAD diet. That said, applying it effectively requires personalization. The right plan adapts the science to your food preferences, lifestyle, and daily routine so it’s sustainable long term, while ensuring you’re getting the right nutrients in the right amounts and pairings to support your heart, brain, bone, gut, and functional aging.
Is coffee bad for peripheral artery disease?
Moderate coffee consumption isn’t considered harmful for most people with PAD and may even have cardiovascular benefits due to its polyphenol content.
Are eggs okay with peripheral artery disease?
For most people with PAD, eggs can be part of a heart healthy diet. However it depends on how many you’re eating, what else you’re consuming throughout the day, and whether you’re a cholesterol hyperabsorber. Some people are genetically more sensitive to dietary cholesterol and may see a greater impact on their LDL levels, which is another reason why personalized guidance based on your individual labs matters.
Can PAD be reversed with diet and exercise?
Diet and exercise can meaningfully improve PAD symptoms, slow plaque progression in the femoral arteries, improve blood flow, and reduce your overall cardiovascular risk. But the results depend entirely on how targeted and personalized your approach is. Generic healthy eating advice won’t move the needle the way a science based nutrition plan tailored to your specific labs, nutrient needs, and cardiovascular risk factors will.
What foods should you avoid with peripheral artery disease?
Foods to avoid with peripheral artery disease are those that worsen inflammation, raise atherogenic LDL cholesterol, and accelerate plaque progression. The worst foods for PAD include saturated fats, trans fats, processed and red meats, refined sugars, and ultra-processed foods. Limiting these while consistently adding in the right nutrients is what makes the biggest difference for your long term vascular health.
About the Author
Michelle Routhenstein is a Registered Dietitian Nutritionist, Preventive Cardiology Nutritionist, and Certified Diabetes Educator with over 14 years of experience specializing in cardiovascular nutrition. As the owner of Entirely Nourished, she takes a nutrient first, science based, and personalized approach to the prevention and management of heart disease.
Michelle has helped thousands of people transform their cardiovascular health by addressing the root causes of heart disease rather than just the symptoms. Her clients have lowered their blood pressure and cholesterol, improved heart function, put Afib into remission, reduced insulin resistance, lost abdominal weight, and meaningfully reduced their risk of heart attacks and strokes. Many have even been able to reduce or eliminate their heart medications entirely through her science based, personalized approach.
If you’re ready to go beyond generic advice and get a deep understanding of how to protect your heart through personalized, science based nutrition, join the interest list for Optimize, her 6-week live group program. You’ll walk away knowing exactly what to eat, why it matters, and how to make it work for your specific labs and health history. Join here.
References
- Zemaitis MR, Boll JM, Kato M, et al. Peripheral Arterial Disease. [Updated 2026 Jan 31]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK430745/
- Poznyak, A. V., Litvinova, L., Poggio, P., Sukhorukov, V. N., & Orekhov, A. N. (2022). Effect of Glucose Levels on Cardiovascular Risk. Cells, 11(19), 3034. https://doi.org/10.3390/cells11193034
- Senoner, T., & Dichtl, W. (2019). Oxidative Stress in Cardiovascular Diseases: Still a Therapeutic Target?. Nutrients, 11(9), 2090. https://doi.org/10.3390/nu11092090
- Cecchini, A. L., Biscetti, F., Rando, M. M., Nardella, E., Pecorini, G., Eraso, L. H., Dimuzio, P. J., Gasbarrini, A., Massetti, M., & Flex, A. (2022). Dietary Risk Factors and Eating Behaviors in Peripheral Arterial Disease (PAD). International journal of molecular sciences, 23(18), 10814. https://doi.org/10.3390/ijms231810814
- Milena, E., & Maurizio, M. (2025). Exploring the Cardiovascular Benefits of Extra Virgin Olive Oil: Insights into Mechanisms and Therapeutic Potential. Biomolecules, 15(2), 284. https://doi.org/10.3390/biom15020284
- Tangney, C. C., & Rasmussen, H. E. (2013). Polyphenols, inflammation, and cardiovascular disease. Current atherosclerosis reports, 15(5), 324. https://doi.org/10.1007/s11883-013-0324-x
- Norouzzadeh, M., Hasan Rashedi, M., Ghaemi, S., Saber, N., Mirdar Harijani, A., Habibi, H., Mostafavi, S., Sarv, F., Farhadnejad, H., Teymoori, F., Khaleghian, M., & Mirmiran, P. (2025). Plasma nitrate, dietary nitrate, blood pressure, and vascular health biomarkers: a GRADE-Assessed systematic review and dose-response meta-analysis of randomized controlled trials. Nutrition journal, 24(1), 47. https://doi.org/10.1186/s12937-025-01114-8
- Emdin, C. A., Anderson, S. G., Callender, T., Conrad, N., Salimi-Khorshidi, G., Mohseni, H., Woodward, M., & Rahimi, K. (2015). Usual blood pressure, peripheral arterial disease, and vascular risk: cohort study of 4.2 million adults. BMJ (Clinical research ed.), 351, h4865. https://doi.org/10.1136/bmj.h4865