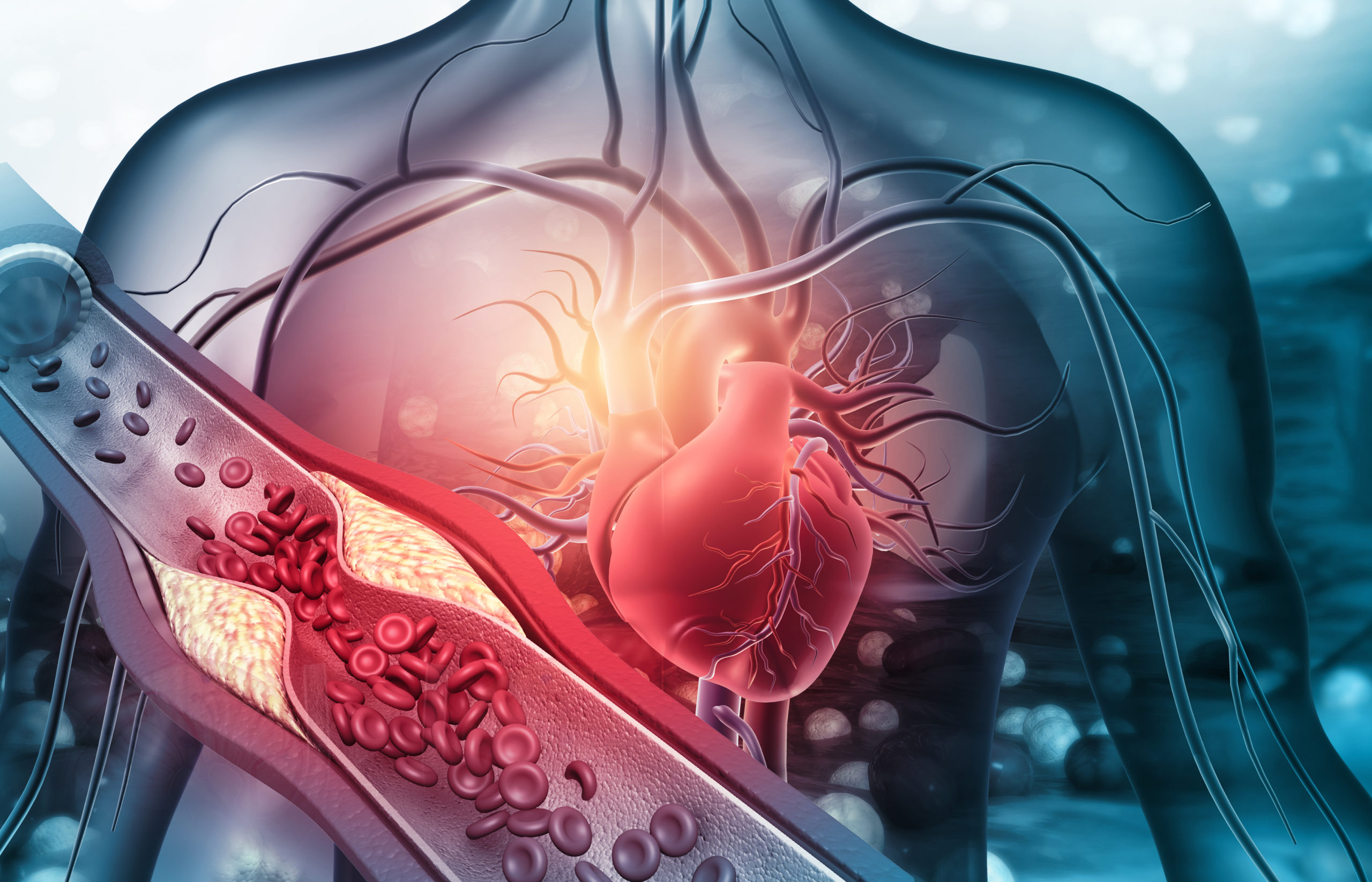
Understanding all of the numbers in your cholesterol tests can be confusing. You want to lower your risk for atherosclerosis, or even reverse it if you can. This article will tell you the most important cholesterol numbers to watch, how atherosclerosis forms, and what you can do to reduce your risk. (To learn more about atherosclerosis and cardiovascular disease, check out the article What is a Cardiac Diet?)
What the LDL Particle Number Is, What It Means, and Why It Matters
Low Density Lipoproteins (LDL) particles are like buses carrying cholesterol and triglycerides in your bloodstream. On your blood test, the LDL number is the amount of cholesterol in the LDL buses in your blood. For years, LDL has been called “bad cholesterol” and a marker for atherosclerosis risk.
However, as scientists research and learn more, they are now looking at the number and size of the LDL particles (those LDL buses) in the bloodstream and how they are associated with atherosclerosis risk. In fact, the latest research is showing that the number of LDL particles (LDL-P), or the number of LDL buses, in your bloodstream has a stronger association with atherosclerosis risk than the amount of cholesterol those buses carry (LDL)1 .
Your LDL particle number matters because the more LDL buses in your bloodstream, the more likely that those buses can move into the walls of your blood vessels. When this happens, the cholesterol they are carrying goes into the blood vessel walls which can then lead to plaque development in the walls of your blood vessels.
How To Find Out Your LDL Particle Number
As research gives us more information about what is going on with the cholesterol carriers (the buses) in our blood and the role they play in the development of atherosclerosis, more advanced cholesterol tests have been developed. Using this more advanced testing gives you more information about what your risks are so you can take action to reduce them.
The LDL particle number is one piece of an advanced lipid test your doctor can order. In fact, an advanced lipid test will give you the following information that can be used to further understand your risk for developing atherosclerosis:
- LDL particle number
- LDL particle size
- LDL pattern
- Lipoprotein (a)
- ApoB
Why LDL Particle Size Matters
Along with knowing your LDL particle number, knowing the LDL particle size will provide even more information about your risk for developing atherosclerosis. Although LDL has been branded as “bad” cholesterol, not all LDL particles are created equal.
Your LDL particles can be large, medium, or small. The small LDL particles are associated with a greater risk of developing atherosclerosis. This test result is reported as Pattern A or Pattern B. Pattern B indicates that more small LDL particles are present, which means they are more likely to enter the arterial wall and cause plaque formation.
Why ApoB Matters
ApoB is another marker to watch if you’re concerned about developing atherosclerosis. Although you may not have heard of ApoB before, research is showing it has a large role in the development of atherosclerosis.
ApoB is a molecule on some of the LDL cholesterol molecules, think of it like a flag that some of the buses have and some don’t. That ApoB flag means that that LDL bus is one that is highly associated with the development of atherosclerosis, much more so than the buses without the ApoB flag. The more ApoB flags, the greater the risk of atherosclerosis developing.
To understand how LDL particle number, LDL particle size, and ApoB play a role in atherosclerosis, we’ll look at how atherosclerosis forms.
The 4 stages of the Development of Atherosclerosis
Atherosclerosis develops over a period of years and goes through 4 stages. Understanding these stages will help you understand how you can reduce your risk of developing atherosclerosis.
Stage 1: Endothelial Cell Injury
Endothelial cells are specialized cells that line your heart and blood vessels. There is only one layer of these cells in your blood vessels. Depending on where the blood vessels are, there are layers of other cells underneath them.
In the smallest capillaries, your blood vessels are only one layer of endothelial cells thick. This allows oxygen and nutrients to move out of the blood vessels to the cells, and waste like carbon dioxide to move out of the cells into the blood vessels2.
Your endothelial cells can be injured, which is the first step in the development of atherosclerosis. The injury can be from the pressure of the blood moving through the vessels, surgery, or an immune response3. You could think of it as a scrape or cut on your arm, but in your blood vessels.
Those at greater risk of endothelial injury are those with one or more chronic, uncontrolled conditions such as:
- High blood pressure, also known as hypertension
- Diabetes, insulin resistance, or uncontrolled high blood sugar
- High LDL cholesterol, or triglycerides
- Chronic kidney failure
Smoking also increases the risk of developing endothelial injuries4.
Unfortunately, the first thing that happens with an injury to your endothelial cells isn’t a scab. Cholesterol starts to collect in the injury in what is technically called lipoprotein deposition.
Stage 2: Lipoprotein Deposition
After endothelial cells are injured, those LDL buses we talked about earlier get into the injury and release the cholesterol they are carrying. Researchers think this is why the LDL particle number is important.
If there are more LDL buses in the bloodstream, there’s a greater chance that they’ll be close by when the injury happens. The more LDL buses in the bloodstream, the more likely they’ll be there, ready to make a stop and drop off their cholesterol.
Those small LDL particles along with those LDL particles with ApoB are on alert for any endothelial injury, much more so than medium or large LDL and those without ApoB. As soon as they detect an injury they are going in and dropping off their cholesterol loads.
This cholesterol deposition starts and develops a fatty streak where the injury occurred. Along with cholesterol being deposited, inflammation starts where the injury occurred.
Stage 3: Inflammation
Inflammation is when your immune system gets called into action. In relation to atherosclerosis, inflammation starts when there is an endothelial injury. Just like the LDL buses in your bloodstream, you have immune cells also circulating looking for injuries.
When the circulating immune cells spot the endothelial injury, they stay there to start working on it, and send out a call for help from other parts of the immune system.
Depending on the damage, how much cholesterol gets into the injury and the immune system response, the fatty streak can be tiny or large. Repeated injuries in the same area, or development of a large fatty streak can cause the blood vessel to be narrowed to the point of being blocked.
The cholesterol and immune cells are what make up the plaque in the walls of your blood vessels you’ve probably heard about.
Once the immune system has the injury under control, a fibrous cap develops.
Stage 4: Creation of a Fibrous Cap
The final stage of stabilizing the injury is the development of a fibrous cap. The fibrous cap is made up of fibrous tissue, hence the name.
The goal of developing the cap is to stabilize the cholesterol and immune cells that are repairing the initial endothelial injury. It is kind of like a scab that develops over a cut except imagine that the cut is swollen and the cap forms over the swollen area.
If the cap weren’t developed, the plaque would remain unstable and could potentially come loose and cause a clot that can block blood vessels, arteries, and cause a heart attack (a myocardial infarction) or stroke5.
Development of the fibrous cap takes time. Once it has formed, over time, it hardens. If the cap isn’t hardened, it can break off and cause the same things that happen when an unstable plaque becomes loose, as mentioned above.
The end result of this process is that, where the injury happened, your blood vessel is now narrower than it was originally. The blood vessel is also more stiff and less flexible due to the plaque and cap. All of this buildup is known as atherosclerosis.
Now that you know how atherosclerosis develops, let’s talk about if it can be reversed.
Can Atherosclerosis Be Reversed?
Atherosclerosis is a process that happens in your body as you age. Depending on lifestyle and genetic factors, the plaque can accelerate at a younger age and more aggressively than others. By halting the progression early by adhering to a truly science based heart healthy diet and lifestyle, we can halt its progression.
Once the plaque and fibrous cap have developed, they won’t go away. I know that isn’t the answer you wanted to hear. What you can do, however, is take proactive steps to reduce your risk of developing more endothelial cell injuries and fatty deposits which may reduce your risk of developing more plaque formation in the arteries.
A surgical procedure called an angioplasty, often with stent placement, can open blood vessels that have been fully or partially blocked due to atherosclerosis. (I’ll have a blog post on this soon). Keeping the stent and other blood vessels open by optimizing your blood vessel health and addressing all of these 4 stages can avoid more plaque development.
What You Can Do to Now Reduce Your Risk of Developing Atherosclerosis
You’ve probably read articles that tell you about increasing your intake of fruits, vegetables, beans, legumes, olive oil, and lean proteins you eat. They’ll also tell you about increasing time spent moving and decreasing time spent sitting every day.
All of those things are true! They can help.
Also, getting any chronic, uncontrolled conditions under control can reduce your risk, as does stopping smoking if you’re a smoker.
To really get to the bottom of atherosclerosis, we need to understand each of the four steps talked about above, and optimize your blood vessel health.
I created my 6-week heart optimization group program in order to optimize your blood vessel health to truly reduce your risk of heart attacks. This program is jam-packed with science based nutrition and lifestyle behavior change recommendations geared to optimize your heart health and prevent/halt atherosclerosis promotion. It also addresses achieving optimal laboratory parameters, reducing your modifiable heart disease risk factors, and makes you more confident in your nutrition and lifestyle choices. To learn more about my group program and apply for the next cohort, click here.
** This article is for informational purposes only and not a substitute for individualized medical advice or treatment. Always seek the advice of a qualified health professional with any questions you may have regarding your health.
References
4Healthwise Staff. (2020b, August 31). Atherosclerosis | Michigan Medicine. University of Michigan Health Michigan Health. Retrieved February 3, 2022, from https://www.uofmhealth.org/health-library/ue4664abc
5Watson, M. G., Byrne, H. M., Macaskill, C., & Myerscough, M. R. (2018). A two-phase model of early fibrous cap formation in atherosclerosis. Journal of Theoretical Biology, 456, 123–136. https://doi.org/10.1016/j.jtbi.2018.08.010