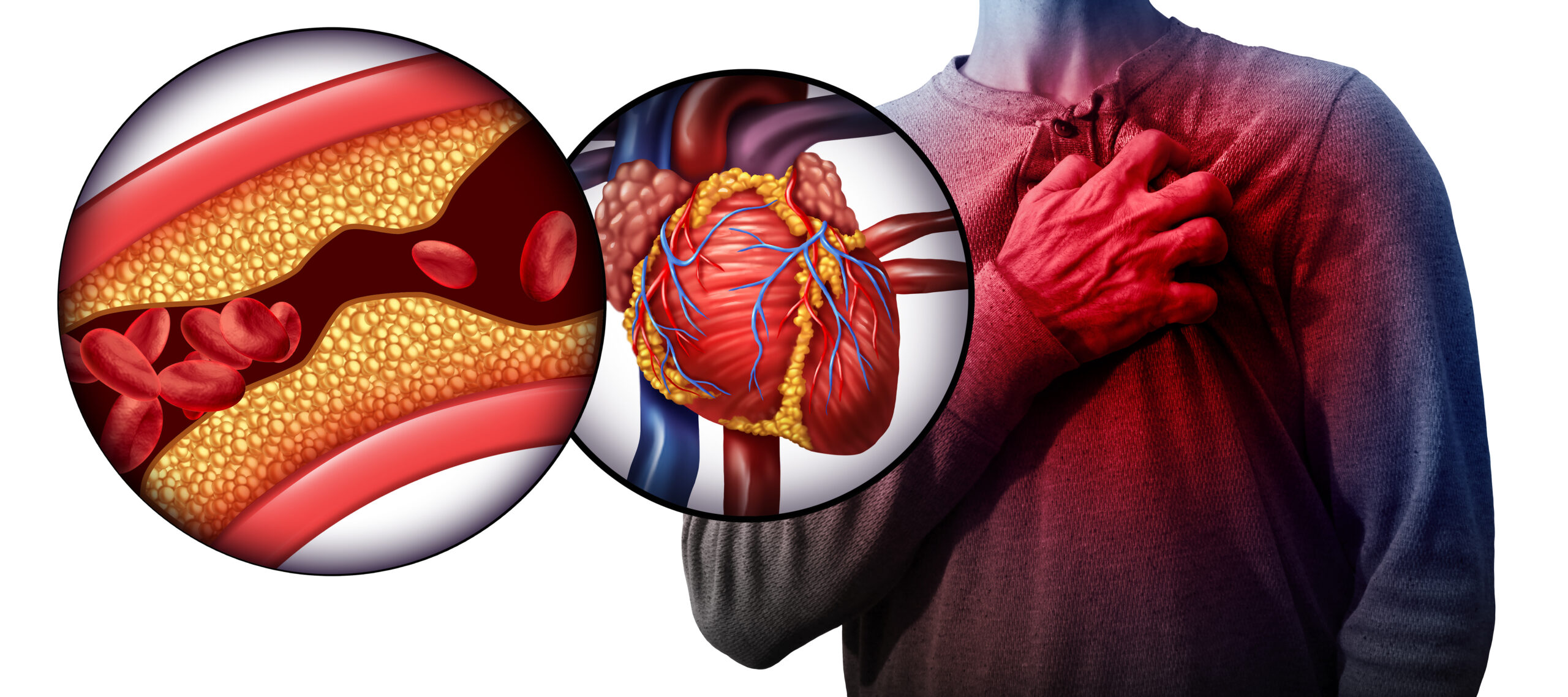
A “widowmaker” heart attack — more formally known as an anterior ST-segment elevation myocardial infarction (STEMI) — is a frightening term for a type of heart attack that occurs when the main artery supplying blood to the heart becomes almost completely blocked.
It gets its name because it’s so severe that, without immediate treatment, it often proves fatal. This can be overwhelming to understand, but it’s important to know that with prompt medical care, widowmaker heart attack prognosis can be improved and lives can be saved.
How serious is a widowmaker heart attack?
Widowmaker heart attack prognosis depends on how quickly one can get medical attention. The 30-day mortality rate for a widowmaker heart attack is between 2.5 to 10%, with the mortality rate being slightly higher for women than men.
Unfortunately, many people who suffer from a heart attack do not know they’re at risk.
This was the same exact case for my client, who is a 40-year-old man who had a widowmaker heart attack while on a run. He had no past medical history and he participated avidly in CrossFit.
After his heart attack, he joined my 3-month VIP nutrition individual program and we worked closely together to optimize his nutrition to improve his cardiovascular function (his ejection fraction was 30% post-heart attack, indicating heart failure), improve his laboratory values (LDL was 138mg/dL and BP was 154/99mmHg) and reduce his risk of a future event.
In 3 months, he had increased his ejection fraction to 47%, his BP average was 117/76mmHg, and his cardiac rehab center asked him to be part of the testimonial advertisement because they have never seen such significant positive change in strength and recovery in such a short period.
My client attributed a lot of this to being nutrient-sufficient and addressing the underlying root cause with proper science-based nutrition.
I received an email from him 6 months after he completed the program, saying: “Hi Michelle, just an update. All doing great. My EF is now at 61% and all the readings are good. I’m also off of my beta blockers and statin. My bad cholesterol went from 138 to 28 it’s been amazing how my food intake has transformed it all. Thank you.”
Widowmaker Symptoms, Causes, and Risk Factors
What are the symptoms of a widowmaker heart attack?
Widowmaker symptoms are similar to other heart attacks. A widowmaker heart attack can include one or more of the following symptoms:
- Pain or discomfort in the neck, jaw, back, arms, or stomach
- Shortness of breath
- Chest pain, tightness, or discomfort
- Lightheadedness, weakness, or feeling faint
- Breaking out in a cold sweat
- Nausea
What causes a widowmaker heart attack?
A widowmaker occurs when the left anterior descending (LAD) artery is completely blocked after a plaque rupture. Plaque in the LAD can be seen on a Coronary Calcium (CAC) scan, which is a helpful tool for monitoring the health of your arteries and risk for a widowmaker heart attack (and can provide a life-saving widowmaker calcium score).
The LAD artery supplies oxygenated blood to the interventricular septum between the left and right ventricles of the heart as well as the anterior left ventricle. The LAD artery can become subject to arterial plaque buildup which can cause narrowing and stiffness in the artery.
Arterial plaque results from cholesterol, cellular waste, fatty substances, and fibers building up along the inner arterial wall. Eventually, due to inflammation, oxidation, stress, and weakening of the plaque structure, an arterial plaque can rupture and cause a blockage to the arteries, also known as coronary thrombosis.
Because the LAD artery is responsible for bringing oxygenated blood to half of the heart, a blockage can result in inadequate blood flow, myocardial injury, and even disruptions in the heart’s normal contraction.
Understand your risk factors
Despite its moniker of the “widowmaker,” a STEMI can affect anyone. Men are more likely to have a widowmaker heart attack than women, but the outcomes can differ greatly.
The American Heart Association recognizes several risk factors that can increase a person’s risk for a widowmaker heart attack:
- Diabetes
- Hypertension
- Smoking
- Stress
- Weight
- Family history of coronary heart disease
- Dyslipidemia (an imbalance of cholesterol and/or triglycerides)
- Age – men aged 45 years and older and women aged 55 years and older are at higher risk
How to Prevent a Widowmaker Heart Attack
Whether you’re hoping to avoid an initial widowmaker heart attack or a recurrent one, prevention is essential. Optimizing your everyday lifestyle habits and utilizing preventive cardiovascular screens is key.
Preventive screenings
Individuals who are at risk for heart disease between the ages of 40-70 years, and those with a family history of high cholesterol, can benefit from calcium-score screening.
A CAC scan uses a CT scan to provide pictures of your heart’s arteries and calculates calcium deposits present in the heart. Is there a widowmaker calcium score? Not definitively, but a higher calcium score may indicate a plaque buildup and an increased risk for a heart attack. If significant plaque buildup is found in the LAD, then this may indicate the potential for a widowmaker heart attack.
Heart-healthy diet
Unfortunately, many individuals who have had a heart attack or are at an increased risk for one are prescribed a pretty generic “heart-healthy diet” with no personalized or detailed recommendations. Let’s unpack what this really means and why nutrition is so effective for improving heart health.

A great number of different food patterns like a plant-based diet or Mediterranean diet can be protective against a widowmaker heart attack. At the root of all things, a heart-healthy diet is one that is well-balanced in macronutrients, micronutrients, and therapeutic foods to help your heart work optimally.
Research shows that high-quality diets consisting of a variety of foods significantly reduce the risk of heart disease. Beyond providing vitamins, minerals, and macronutrients, various foods have compounds that give additional health benefits.
For instance, plant polyphenols are phytochemicals that can support healthy blood vessels, normal cholesterol levels, and protect against inflammation. Some examples of polyphenols that have been well-studied for their impact on heart health include resveratrol in black grapes, epigallocatechin gallate (EGCG) from tea, curcumin in turmeric, and quercetin in red onions.
Plant sterols and stanols are plant substances that are structurally similar to cholesterol. They are effective for managing cholesterol levels due to their ability to inhibit the absorption of cholesterol by the body.
Phytoestrogens like lignans and isoflavones from flaxseed and soy, respectively, can also protect women from cardiovascular disease. They have antioxidant and anti-inflammatory benefits, may help lower high cholesterol, improve endothelial health, and support hormonal balance.
The fiber in plant foods is important for supporting healthy blood sugar regulation and increasing insulin sensitivity. Insulin resistance increases your risk of type 2 diabetes, which is a major risk factor in cardiovascular disease. Eat a variety of fiber-rich foods like legumes, leafy greens, berries, cruciferous vegetables, and whole grains.
To get the most out of your diet, focus on adding in nutrient-rich therapeutic foods your body needs to achieve improved blood pressure control, reduced inflammation and oxidative stress, increased insulin sensitivity, and overall improved heart function.
Eating for heart health is a lifelong plan and should be sustainable for you. It’s important to work with a registered dietitian knowledgeable in cardiovascular health. I discuss all of these foods and how to balance it appropriately in my 6-week Heart Health Optimization group program.
Exercise
Regular exercise can support the flexibility of your arteries and reduce the risk of atherosclerosis. Current guidelines recommend that healthy adults get at least 150-300 minutes of moderate- to vigorous-intensity exercise weekly plus strength training twice a week.
Two types of exercise that are shown to be effective for heart health include aerobic (cardio) and resistance (strength) exercises. Aerobic exercises include exercises that use large muscle groups and are maintained for a while, including running, hiking, swimming, dancing, and biking. Resistance exercises are typically done for shorter durations of time and include some weight resistance such as weight lifting, squats and lunges, push-ups, and similar exercises.
Studies find that doing both resistance and aerobic exercise in your routine may be the most effective for losing weight, improving cardiorespiratory fitness, and increasing fat loss compared to resistance or aerobic exercise alone.
Medication
Taking medications as needed and as prescribed for normal blood clotting, blood pressure, and blood lipid levels can reduce the risk of further heart disease and complications. Never add, adjust, or stop medications without consulting with your provider.
If choosing to add supplements to your diet, you should always consult with your healthcare team including your Registered Dietitian Nutritionist who specializes in heart disease to ensure it’s personalized for you, is providing benefit versus potential harm, and takes into account your medical history, diet, and medications you use.
Monitoring labs
Along with CAC scans, keeping up to date with your medical labs can help you know when to seek additional support. Important labs to monitor during your regular doctor’s visits include blood pressure, hsCRP, LDL (advanced if available), triglycerides, and hemoglobinA1c, to name a few.
I created a self-paced course to help you learn more about the other lab tests that may help you better assess your heart health.
Weight management
Managing your weight can reduce your risk of heart attack and other chronic conditions that can cause damage to your vascular system. People with a BMI of 25 or higher generally have a greater risk of getting a widowmaker heart attack. Losing 5-10% of your body weight can significantly reduce certain cardiovascular risks like triglyceride levels, LDL, and total cholesterol.
In addition to managing your overall weight, where your weight settles has an impact on your cardiovascular risk. Waist circumference is an anthropometric measurement that correlates with visceral adiposity, or fat that surrounds the internal organs. A higher waist circumference is associated with a great risk of metabolic disease because this type of fat is more metabolically active and is usually associated with inflammation and insulin resistance.
The current guidelines for waist circumference notes that a waist circumference >102 cm (40 in) in men or >88 cm (35 in) in women is associated with greater health risks. However, these guidelines are not universal, and waist circumference thresholds may differ based on BMI category and ethnicity.
Smoking cessation
Smoking is a major risk for the development of arterial plaques and heart attacks. Smoking damages the blood vessels, decreases blood flow and oxygen delivery to the heart, and increases inflammation, which can promote plaque formation.
Research shows that female smokers have a 25% higher risk of developing coronary heart disease than men with the same exposure to tobacco smoke. Fortunately, smoking cessation is one of the most impactful things you can do to protect your heart health and lower your risk of a heart attack.
Diabetes management
Diabetes is a risk factor for heart attacks due to its impact on the health of your vascular system. Excess blood glucose can decrease the elasticity of your blood vessels, reduce blood flow, and increase high blood pressure risk.
Managing your blood sugar through diet, exercise, and prescribed medications as needed can minimize the damage to the blood vessels and arteries of your heart.
Widowmaker Heart Attack: Final Thoughts
While a widowmaker heart attack is very dangerous, there are many things you can do to help lower your risk of ever experiencing one. Never underestimate the power that science-based nutrition and optimized lifestyle habits can have on your cardiovascular health, no matter what they look like today. It’s never too late to make these changes, especially if you’re concerned about your risk factors.
As a cardiovascular dietitian, I’m ready to help you come up with a personalized plan to protect your heart health. Click here to schedule a discovery call with me to talk through our options for working together.
References
- Akbar H, Foth C, Kahloon RA, et al. Acute ST-Elevation Myocardial Infarction. [Updated 2023 Jul 31]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK532281/
- Cenko E, Yoon J, Kedev S, et al. Sex Differences in Outcomes After STEMI: Effect Modification by Treatment Strategy and Age. JAMA Intern Med. 2018;178(5):632-639. doi:10.1001/jamainternmed.2018.0514
- American Heart Association. (2022). Warning Signs of a Heart Attack. Retrieved from: https://www.heart.org/en/health-topics/heart-attack/warning-signs-of-a-heart-attack
- Palasubramaniam J, Wang X, Peter K. Myocardial Infarction-From Atherosclerosis to Thrombosis. Arterioscler Thromb Vasc Biol. 2019;39(8):e176-e185. doi:10.1161/ATVBAHA.119.312578
- American Heart Association. (2022). Understand Your Risks to Prevent a Heart Attack. Retrieved from: https://www.heart.org/en/health-topics/heart-attack/understand-your-risks-to-prevent-a-heart-attack
- Petersen KS, Kris-Etherton PM. Diet Quality Assessment and the Relationship between Diet Quality and Cardiovascular Disease Risk. Nutrients. 2021;13(12):4305. Published 2021 Nov 28. doi:10.3390/nu13124305
- Khurana S, Venkataraman K, Hollingsworth A, Piche M, Tai TC. Polyphenols: benefits to the cardiovascular system in health and in aging. Nutrients. 2013;5(10):3779-3827. Published 2013 Sep 26. doi:10.3390/nu5103779
- Trautwein EA, Vermeer MA, Hiemstra H, Ras RT. LDL-Cholesterol Lowering of Plant Sterols and Stanols-Which Factors Influence Their Efficacy?. Nutrients. 2018;10(9):1262. Published 2018 Sep 7. doi:10.3390/nu10091262
- Rietjens IMCM, Louisse J, Beekmann K. The potential health effects of dietary phytoestrogens. Br J Pharmacol. 2017;174(11):1263-1280. doi:10.1111/bph.13622
- Yang YJ. An Overview of Current Physical Activity Recommendations in Primary Care. Korean J Fam Med. 2019;40(3):135-142. doi:10.4082/kjfm.19.0038
- Patel H, Alkhawam H, Madanieh R, Shah N, Kosmas CE, Vittorio TJ. Aerobic vs anaerobic exercise training effects on the cardiovascular system. World J Cardiol. 2017;9(2):134-138. doi:10.4330/wjc.v9.i2.134
- Schroeder EC, Franke WD, Sharp RL, Lee DC. Comparative effectiveness of aerobic, resistance, and combined training on cardiovascular disease risk factors: A randomized controlled trial. PLoS One. 2019;14(1):e0210292. Published 2019 Jan 7. doi:10.1371/journal.pone.0210292
- Brown JD, Buscemi J, Milsom V, Malcolm R, O’Neil PM. Effects on cardiovascular risk factors of weight losses limited to 5-10. Transl Behav Med. 2016;6(3):339-346. doi:10.1007/s13142-015-0353-9
- Ross R, Neeland IJ, Yamashita S, et al. Waist circumference as a vital sign in clinical practice: a Consensus Statement from the IAS and ICCR Working Group on Visceral Obesity. Nat Rev Endocrinol. 2020;16(3):177-189. doi:10.1038/s41574-019-0310-7
- Gallucci G, Tartarone A, Lerose R, Lalinga AV, Capobianco AM. Cardiovascular risk of smoking and benefits of smoking cessation. J Thorac Dis. 2020;12(7):3866-3876. doi:10.21037/jtd.2020.02.47